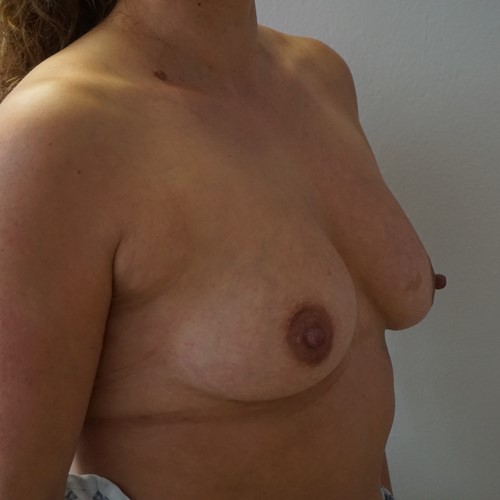
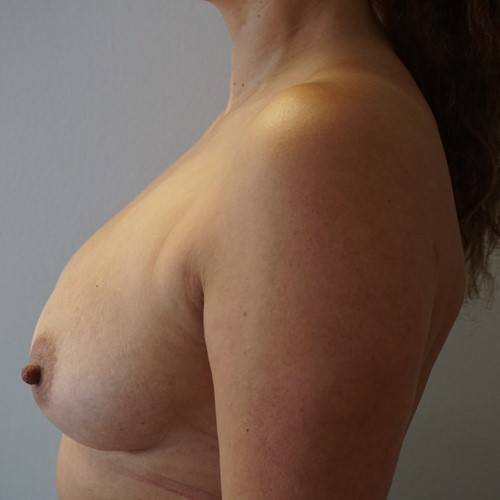
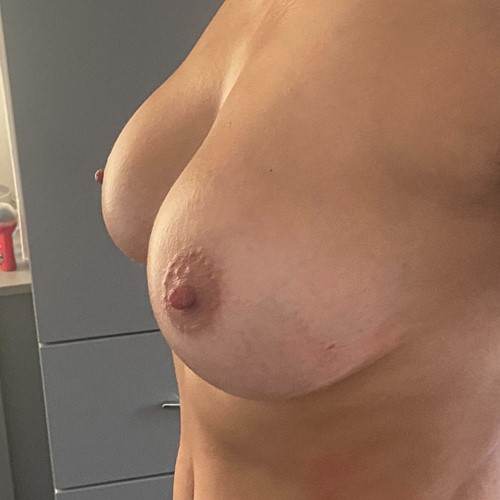
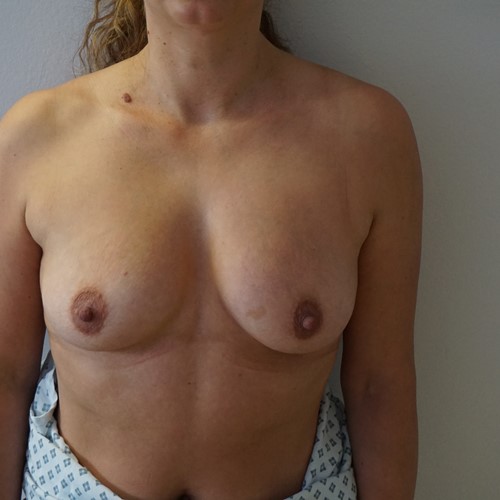
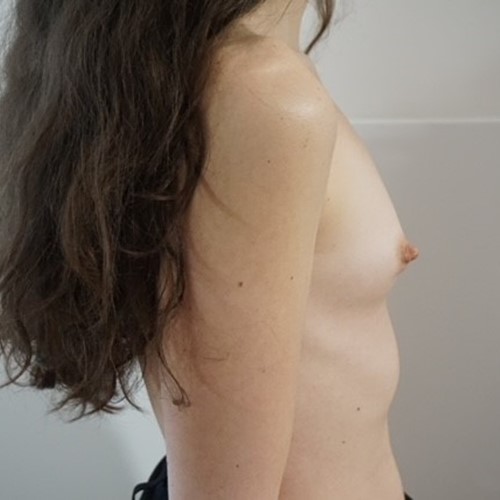
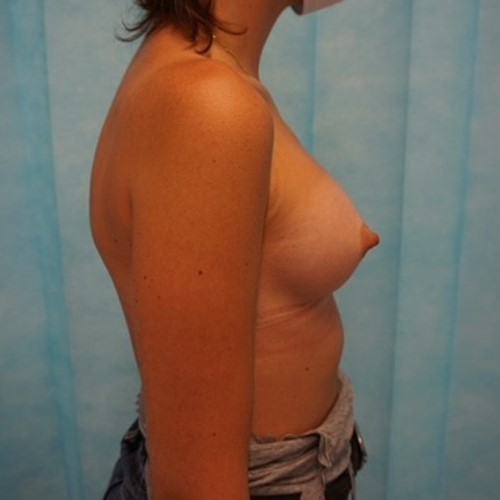
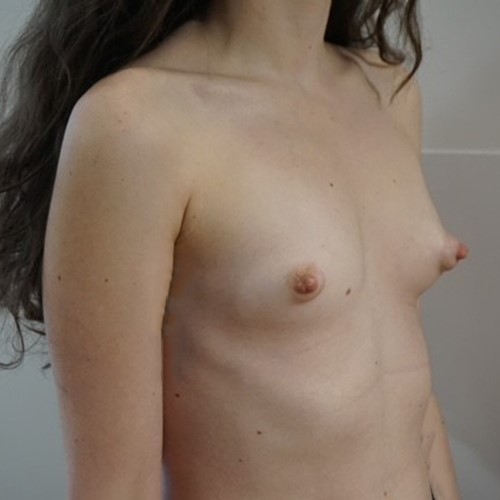
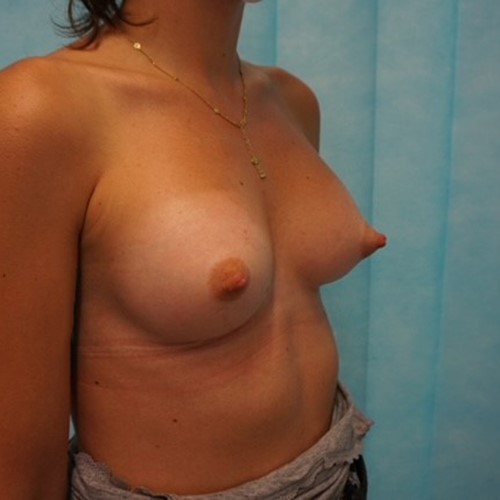
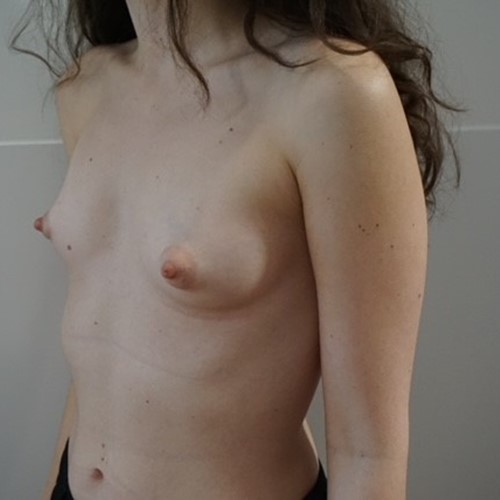
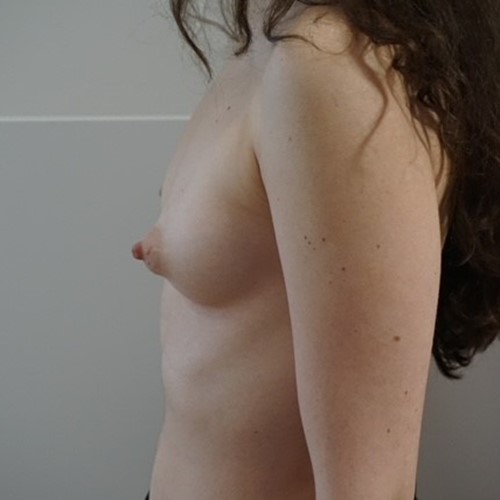
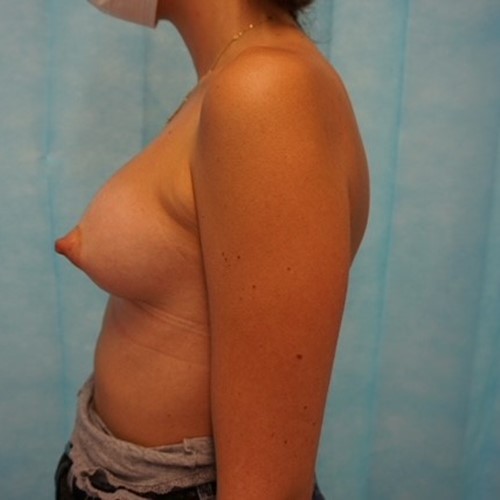
Most women have some minor degree of breast asymmetry. In some women breast asymmetry may be extreme, while others may have a particular condition such as Poland's syndrome or tuberous breasts. Differential breast augmentation, or tissue expansion can be used to correct asymmetry. In addition, breast implants can be inserted as one form of breast reconstruction following mastectomy for cancer.
A breast augmentation procedure always leaves a scar (the implant has to be inserted through an incision), although this usually becomes inconspicuous with time. Mr Soldin uses an incision placed under the breast which leaves a well hidden scar.
All patients develop a thin capsule (scar) around the implant. In most cases this is thin, pliable and not noticeable. Some patients will, however, with time, develop a capsular contracture months or years after the surgery which can leave the breasts hard and misshapen. In this group of patients, the capsule may require removal and the implant may need replacing. It is important to know that when you make the decision to have a breast augmentation, you understand that further breast surgery in the future is likely e.g. to replace ruptured implants, or for attention to a capsular contracture.
Despite these potential problems, breast augmentation remains one of the best plastic surgery operations and most patients are very happy. The surgery is quick and safe, the results predictable and immediate and the recovery quick and relatively pain free.
Initial Consultation
At your first visit, your suitability for the procedure and your fitness for surgery will be assessed. Your breasts will be examined. If your breasts are sagging, a breast lift (mastopexy) may be recommended.
It is frequently difficult to decide on what size implant is required. Women will often state that they want to go from a B to a C cup, but this does not help in deciding what size implant you will need. Bra manufacturers frequently vary in what they define as a particular cup size and one manufacturer's C cup might be another's B or D cup. Surgeons define implant size in millilitres (1 ml = 1 gram) and a typical implant in my practice is between 200 and 290 ml. Although looking at pictures of women with similar breasts to yours and what you want may be helpful, there are also pitfalls with this method. Putting a sizer in the bra is also helpful although, again, once implanted under your breast, the effect may be slightly different. A silk sock filled with rice to your required breast size can make a useful sizer and allows you to measure at home what volume you want. This helps your surgeon understand the approximate size you are looking for.
Currently there is some debate regarding conventional vs. anatomical implants. Anatomical implants are teardrop shaped: thinner above and thicker below. They need to be placed precisely - if they rotate their effect is the exact opposite of what is intended. Anatomical implants are about one and a half times pricier than conventional implants. I believe that most women need a bit of volume above (especially older patients with empty breasts). I also believe that breast shape is not much affected by implant shape and it is not my current practice to use anatomical implants. Round implants are safer to use in my view.
Preoperatively it is important that you understand the procedure and what it can achieve. You should be aware of the risks and complications. All your questions should be answered. A well-prepared patient will do better with surgery and will be more satisfied with the final result. Mr Soldin aims for a natural look. The ‘fake’ or ‘stuck on’ look is not natural and in Mr Soldin’s opinion more likely to give you trouble in the long run.
Safety of silicone gel-filled implants
The current view of the British Association of Plastic, Reconstructive and Aesthetic Surgeons (BAPRAS), the American College of Rheumatology, the Centre for Disease Control and the American Medical Association is that there is no relationship between silicone breast implants and any chronic disease process, and this view has also been formally expressed by the American Food and Drug Administration (FDA). Of note however is the recent discovery that macro-textured implants can promote the development of ALCL ( Anaplastic Large Cell Lymphoma ).
This newly discovered problem is rare, but still under investigation. It does not seem to occur in smooth walled implants, which is why Mr Soldin is using more of these implants. Silicone gel filled implants still give the most natural look and feel and I believe them to be the best form of augmentation.
Surgery
My usual method of breast augmentation is described below. I will vary this surgery according to patient's individual requirements, but I find the method below provides me with excellent results in the majority of patients. I will give alternative options to my protocol and reasons for doing what I do.
Surgery is usually performed under general anaesthetic as a day case or with a one-night postoperative stay. On arrival on the morning of surgery, you will meet the anaesthetist and I will mark the incision lines and various other landmarks on your skin with a pen. I will also take pre-operative photographs at this stage.
The incision used is a small (about 5 cm) cut under each breast. This incision lies within the natural body crease line and therefore heals up very well. It allows good exposure to create an adequately sized cavity to accept an implant and, very importantly, it allows excellent visualisation of any bleeding points, which can then be controlled. The cavity created is either under the muscle ( if you are slim ) or under the breast ( on top of the muscle). Silicone gel implants are placed through the incision with ease, although saline implants can be inserted via this incision as well. Other incisions (Axillary, Areolar, Umbilical) make the procedure more difficult and longer. Visualisation of the cavity is less good and control of bleeding is less precise. The incision in the armpit can form unsightly scars that may be visible in an evening dress, vests, short sleeves, etc. The incision around the areolae usually provides very limited access, which only allows insertion of saline implants. Incisions in the belly button vastly overcomplicate a relatively simple procedure for very little benefit - the implants frequently are placed too low and the risk of complications is higher.
Through the incision a pocket is created either underneath the breast or underneath the chest wall muscle (so called sub-muscular placement). If you have sufficient breast and subcutaneous tissue then placing the implant right underneath the breast creates a normal looking breast with good cleavage and breast shape. If however you are very thin with not much natural breast tissue or subcutaneous tissue then it is more sensible to place the implant in a sub muscular pocket. This is also associated with a lower capsular contracture rate and still gives a good shape.
Once the subglandular pocket is created, I ensure that any bleeding point is controlled, I wash out the cavity with an antiseptic solution and place the implant. I can use textured surfaced implants as the capsular contracture rate is lower, but these days with ALCL risk,I am also using more smooth walled implants. I use silicone gel filled implants rather than saline implants as the feel and consistency of silicone is infinitely better than saline; the implants do not slosh or wrinkle and I believe that currently there is no better alternative to silicone gel.
Following placement, the incisions are closed with dissolving sutures and a light dressing applied. I sometimes place drains (pipes coming out from under the implant to remove any excess fluid or blood) which stay in for some hours, but try to avoid them if possible.
The surgery takes approximately one and a half hours. After surgery, you will be transferred to the recovery area and then back to the ward.
Post-Operatively
When you awake from surgery in the recovery area, you should be relatively pain free. As the local anaesthetic wears off, you may feel sore, but painkiller medication will be prescribed. On the first postoperative day you should be up and about, and shower. Your breasts will be a little swollen and bruised. The swelling and bruising take about three weeks to settle, but enough of the swelling will be down by the end of the second week to allow you to go shopping for a new bra.
I will see you one week post-operatively for your first visit. Following this, you
Should slowly get back to normal ( about 2 weeks off work, and one month off sport ). Massaging the scar with an aqueous cream helps them to settle.
Some numbness in the breast and particularly the nipple may be noticed for the first few weeks after surgery. Hypersensitivity can also occur. Both are usually transient.
If you have small children at home you will certainly need help for the first week. With regards to driving, I usually advise a similar period ( 1 week ) of no driving but again this is very personal and some people recover very quickly and can get back to driving in a short time. You should be able to return to work within a week or two, depending on the level of activity required by your job. Your breasts will probably be sensitive to direct stimulation for two to three weeks, so you should avoid much physical contact. Physical exercise - begin when you feel ready, generally after four weeks.
Risks and complications
Breast augmentation is a relatively straightforward procedure. As with any surgery, however, there are certain risks and complications. It is important to understand what these are.
- Bleeding
As with any surgical procedure, excessive bleeding following the operation may cause swelling and pain. If excessive bleeding occurs, another operation may be needed to control the bleeding and remove the accumulated blood.
- Infection
A small percentage of women develop an infection around an implant. This may occur at any time, but is most often seen within a week after surgery. A postoperative temperature and local redness, warmth and pain of the breast are signs that may indicate the beginning of an infection. Sometimes this can be controlled with the use of antibiotics, but in other cases the implant may need to be removed. A new implant will be inserted later when the infection has resolved completely ( after about 6 months ).
- Capsular contracture
A Capsule (similar to a scar) develops around every implant and is normal in breast augmentation. Over time this capsule can change and
become harder. This is called a capsular contracture. It is graded 1 – 4. Significant contracture development (grade 3 or 4) is one of the most common complications following breast augmentation. Contracture is usually mild and difficult to feel. It can become more severe, firmer, even hard and painful. We are unsure as to why contracture occurs – Between 10% and 25% of women may develop significant contracture that will require treatment. The risk of developing capsular contracture increases the longer the breast implants are in place.
One of the ways to prevent contracture is to use textured implants that have, overall, about a 50% lower rate of development of significant contracture as compared with smooth implants. Once significant contracture occurs, the treatment is usually with surgery – the implant is exchanged and the capsular contracture either cut (scored) or, sometimes, excised. Some surgeons used to practice a closed capsulotomy by firm manipulation of the breasts with the aim of trying to fracture the capsule. The risk of implant rupture with this technique is high and the procedure is therefore not recommended.
- Sensory changes
Some women report sensory changes: their nipples become oversensitive, under-sensitive, or even numb. You may also notice small patches of numbness near the incisions. These symptoms usually disappear with time, but may be permanent in a few patients.
- Fertility, pregnancy and breast-feeding
There is no evidence that breast implants will affect fertility, pregnancy, or your ability to nurse and breast-feed. If, however, you have nursed a baby within the year before augmentation, you may produce milk for a few days after surgery. This may cause some discomfort, but can be treated with medication.
- Implant rupture
Occasionally, breast implants may leak, tear or rupture. Rupture can occur as a result of injury or compression. Implants do not burst like a balloon – some women have fears that the breast will explode – this does not occur! There is no danger with air travel or deep sea diving.
If a saline-filled implant breaks, the implant will deflate over a few hours to days and the salt water will be harmlessly absorbed by the body.
If a break occurs in a gel-filled implant the silicone gel may be contained by the scar capsule around the implant and you may not detect any change. Many women are walking around with ruptured breast implants and do not know they have had an implant rupture. As long as the silicone is within the capsule there is little risk. Whether any treatment is needed at this stage is controversial. If the silicone gel leaks out of the capsule and into the breast tissue you may detect a change in the shape or firmness of the breast, or a lump. An operation will then be required to replace the broken implant and remove the leaked silicone.
- Breast cancer and breast cancer detection
No clinical studies have shown any evidence of increased risk of breast cancer development in women with implants. In fact most studies show implanted women to have a lower rate of breast cancer development than non-implanted women, possibly because they had smaller breasts and less breast tissue to start with.
Breast implants may however interfere with the detection of breast cancer. Different mammography techniques using special views may be required, and you should explain to the radiologist when the time comes to have a mammogram, that you have breast implants.
While the majority of women do not experience complications, you should make sure that you understand the risks and consequences of breast augmentation.
For many women, the result of breast augmentation can be satisfying, even exhilarating, as they learn to appreciate their new, fuller appearance. Your decision to have breast augmentation is a highly personal one that not everyone will understand. The important thing is how you feel about it. Overall, despite much of the previous media hype around breast augmentation, it is one of the best procedures offered by plastic surgeons and one with a high degree of patient satisfaction.
- ALCL ( Anaplastic Large Cell Lymphoma)
This newly recognised condition is currently under investigation. It is a rare lymphoma which is thought to be related to macro-textured implants. At this time it has not been described in primary breast augmentation using smooth walled implants, which is why Mr Soldin has moved more to using smooth walled implants. It occurs years after the primary operation and presents as swelling in one breast. The curative treatment in most is to remove both the implant and the capsule. Further evidence is awaited.
Checklist
- Make sure I know all the medications you are on before surgery.
- Do not take any aspirin or blood thinning drugs (which include some homeopathic supplements) for at least 2 weeks prior to surgery. Paracetamol is safe.
- Smoking must be stopped at least 6 weeks prior to surgery and afterwards until your wounds have healed.
- Oral contraceptives should ideally be stopped a month prior to surgery but please use some alternative form of contraception.
- Please buy a loose sports bra (one/two sizes up from your current size) and bring this into hospital with you. You will need to wear it day and night for at least 2 weeks after surgery. You must not wear an underwired bra for at least six weeks after your operation.
- Nothing to eat or drink after midnight the night before your operation.
If you are worried post-operatively
Telephone the ward of the hospital from which you have been discharged.
Telephone my secretary Angie Harrison during office hours – 07961221874
In an emergency (and you have failed to contact me by the above two methods) then please telephone St George’s Hospital (020 8672 1255) and ask them to either bleep me or the Resident Plastic Surgery doctor on call (Bleep 7050).